Industry Insight
Unlocking science to discover novel solutions for breast cancer patients
Dr Martina Witzel from Daiichi Sankyo considers the burden of breast cancer highlighting the impact it has on women, and the advances in breast cancer care and precision medicines
Authored by Dr Martina Witzel, head of Oncology Germany at Daiichi Sankyo
“Therapy should be permanently backed up by scientific research without which no progress is possible.” – Marie Curie. (From Marie Curie's speech made at the opening of the Radium Institute in Warsaw, Poland, May 1932.)
Marie Curie is widely regarded as a trailblazer in science. As the laureate of two Nobel Prizes in 1903 and 1911, and the first woman in Europe to obtain a Doctor of Science degree, Curie paved the way for women to enter fields that had previously been held for men only. 1 She was a remarkable woman whose discoveries on radioactivity at the beginning of the 20th century broke new ground for women in science and transformed diagnostic and therapeutic possibilities in oncology and breast cancer. 2 Before the use of radiation in medicine, which was championed by Curie, cancers in many sites were considered to be incurable. While we’ve made huge strides in cancer research over the last century, today, breast cancer remains a significant burden on all of society and particularly women as the world’s most prevalent cancer type. Annually, there are more than two million new cases of breast cancer diagnosed globally and over half a million in Europe alone. 3,4 Sadly, it is estimated that one in seven women in Europe will develop breast cancer before the age of 74. 5 Building on Curie’s legacy, we must continue to invest in scientific research and expand possibilities that relieve the burden for breast cancer patients.
The current treatment paradigm for breast cancer
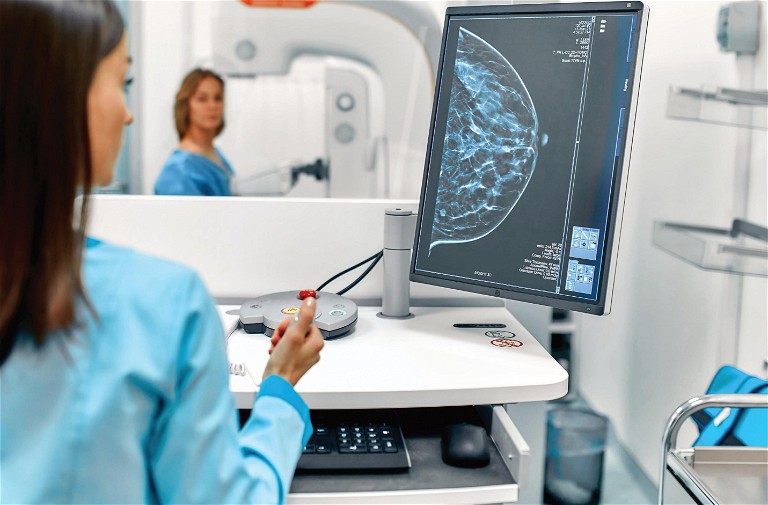
With all cancers, early detection and diagnosis can be fundamental in saving lives. When detected early, the chances of successful treatment and survival from breast cancer can increase. 6 Early diagnosis also means treatment may be less aggressive and have fewer side effects. 7 Data from pre-COVID-19-Europe has shown that early detection programmes were responsible for preventing more than 20,000 breast cancer deaths every year. 8
Early detection ultimately improves cancer survival rates by allowing patients to access care at the earliest possible stage. When early detection is not possible, there is more emphasis on a patient’s treatment plan. Over the last few decades, there have been sizeable breakthroughs in breast cancer care. Through the hard work and dedication of researchers, there are now highly effective new treatments that can provide long-term disease control and management for advanced breast cancer care.9 We’ve also witnessed astounding progress in surgery, radiotherapy, immunotherapy and genetic testing. 10
These advancements have allowed physicians to target and treat breast cancer more precisely, thus considerably improving patient outcomes. In particular, the introduction of precision medicine has been a major leap forward in the fight against breast cancer.
Could precision medicine be the future?
Precision medicine, sometimes referred to as personalised medicine, is an individualised approach to treating and preventing diseases by utilising data from a patient’s medical history, lifestyle, genetic makeup and other factors to develop therapies that are tailored specifically for them. 11,12 By analysing an individual's unique genetic profile, precision medicine can help identify which treatments are most likely to be successful – reducing unnecessary therapies or surgeries as well as improving quality of life. 11 This targeted approach to treatment has enabled doctors to gain a deeper understanding of a patient’s individual cancer, resulting in improved patient outcomes. 13
Powered by scientific research and artificial intelligence (AI), the use of precision medicine is not only advantageous for patients, but also offers benefits to healthcare providers and society as a whole. By drawing on precise data generated from tests such as gene sequencing or imaging scans, doctors can more accurately diagnose diseases and recommend suitable therapies that might not have previously been considered.14 Data from these tests can also provide insights into ways breast cancer can be prevented or detected earlier. 13 This enables clinicians to take steps towards disease prevention rather than responding after symptoms appear later down the line.
The challenges of implementing precision medicine
The potential of precision medicine to revolutionise the way breast cancer is treated has been widely recognised. However, there are still several obstacles to its successful implementation. The cost of treatments is a major factor that can limit access. While the cost of these treatments can vary by location and type of care received, the lack of health insurance coverage in some countries further exacerbates this issue.15,16 There are also infrastructure and resource challenges that need to be addressed for precision medicine treatments to be implemented universally. Many healthcare providers lack the necessary resources or do not have access to the right technology needed for these treatments, whilst navigating large data sets require sufficient computing power which may not always be readily available. 15,17 With the right infrastructure, resources and incentives in place, precision medicine promises to revolutionise healthcare and transform patient lives. These challenges must be addressed for precision medicines to be accessible for all.
“ With the right infrastructure, resources and incentives in place, precision medicine promises to revolutionise healthcare and transform patient lives ”
A look to the future
We are currently living in an era of extraordinary scientific research and innovation in cancer care. Precision medicine is just one example of the breakthrough treatments we’re seeing transform the treatment paradigm. As precision medicine therapies for breast cancer evolve, it is evident that there is immense potential to change the way we approach this disease. Through a commitment to further scientific research and development, we can improve patient lives and advance cancer care. We must never forget Marie
Curie’s legacy and continue to follow the science to unlock the potential of precision medicine and other new therapeutic possibilities.
References
- Visit: sciencedirect.com/science/article/pii/S1507136715001625
- Visit: ncbi.nlm.nih.gov/pmc/articles/PMC3093546/
- Visit: canceratlas.cancer.org/the-burden/europe/
- Visit: iarc.who.int/faq/latest-global-cancerdata-2020-qa/
- Visit: ecis.jrc.ec.europa.eu/pdf/Breast_cancer_ factsheet-Oct_2020.pdf
- Visit: cancer.org/content/dam/CRC/PDF/Public/8579.00.pdf
- Visit: cancer.org/cancer/types/breast-cancer/treatment/treatment-of-breast-cancer-bystage/
treatment-of-breast-cancer-stages-i-iii.html#:~:text=Most%20women%20with%20breast%20cancer,treatment%20you%20will%20likely%20need. - Visit: ncbi.nlm.nih.gov/pmc/articles/PMC7754503/
- Visit: ncbi.nlm.nih.gov/pmc/articles/PMC8886005/
- Visit: news.cancerresearchuk.org/2012/06/03/celebrating-60-years-of-progress/
- Visit:macmillan.org.uk/cancer-informationand-support/treatment/your-treatmentoptions/personalisedmedicine#:~:text=Personalised%20medicine%20uses%20information%20about,is%20sometimes%20called%20precision%20medicine.
- Visit: ncbi.nlm.nih.gov/pmc/articles/PMC7826530/
- Visit: ncbi.nlm.nih.gov/pmc/articles/PMC7272286/
- Visit: ncbi.nlm.nih.gov/pmc/articles/PMC7877825/
- Visit: ascopubs.org/doi/full/10.1200/EDBK_200633
- Visit: efpia.eu/media/589727/unlocking-thepotential-of-precision-medicine-in-europe.pdf
- Visit: ncbi.nlm.nih.gov/pmc/articles/PMC6405506/

Dr Martina Witzel is head of Oncology Germany at Daiichi Sankyo. Dr Witzel obtained her PhD from the University of Würzburg in Germany. She aspires to be an inspirational leader, especially for women in the life sciences sector. With over 27 years of experience in the pharmaceutical industry, Witzel has a diverse background in multiple disease areas (Oncology, Diabetes and central nervous system). She has been focusing on Oncology over the past years in her previous role at Eli Lilly and her current role at Daiichi Sankyo.